
Research
Diabetes Study Favors Surgery to Treat Obese
By DENISE GRADY
Published: January 23, 2008
Weight-loss surgery works much better than standard medical therapy as a treatment for Type 2 diabetes in obese people, the first study to compare the two approaches has found.
Skip to next paragraph
Related
Health Guide: Type 2 Diabetes
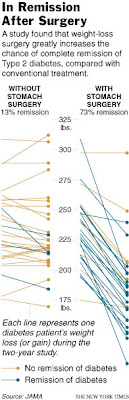
The study, of 60 patients, showed that 73 percent of those who had surgery had complete remissions of diabetes, meaning all signs of the disease went away. By contrast, the remission rate was only 13 percent in those given conventional treatment, which included intensive counseling on diet and exercise for weight loss, and, when needed, diabetes medicines like insulin, metformin and other drugs.
In the study, the surgery worked better because patients who had it lost much more weight than the medically treated group did — 20.7 percent versus 1.7 percent of their body weight, on average. Type 2 diabetes is usually brought on by obesity, and patients can often lessen the severity of the disease, or even get rid of it entirely, by losing about 10 percent of their body weight. Though many people can lose that much weight, few can keep it off without surgery.
(Type 1 diabetes, a much less common form of the disease, involves the immune system and is not linked to obesity.)
But the new results probably do not apply to all patients with Type 2 diabetes, because the people in the study had fairly mild cases with a recent onset; all had received the diagnosis within the previous two years. In people who have more severe and longstanding diabetes, the disease may no longer be reversible, no matter how much weight is lost.
The operation used in the study, adjustable gastric banding, is performed through small slits and loops a band around the top of the stomach to cinch it into a small pouch so that people eat less and yet feel full. Other weight-loss operations are more extreme and involve cutting or stapling the stomach and rearranging the small intestine. Of the 205,000 weight-loss operations performed in the United States last year, 25 percent to 30 percent used the gastric banding.
Remission of Type 2 diabetes after weight-loss surgery is not a new finding; doctors have known about it for years. But the new research is the first effort to find out scientifically how it measures up against medical treatment in similar groups of patients with the disease.
The study reflects a growing interest among researchers in using surgery specifically to treat Type 2 diabetes, even in people who are not as obese as those who typically undergo operations to lose weight. The new thrust is in some sense a measure of desperation, as the United States and the world face increasing rates of the disease and its devastating complications, which can include heart attacks, blindness, kidney failure and amputation. To many doctors, the time is ripe for studying surgery as a potential cure for diabetes, and also as way to understand the disease better and develop better drugs to treat it.
Medical societies in the United States and abroad that once called their specialty bariatric surgery, a term that refers to weight loss, have started adding the word “metabolic” to their titles to emphasize the new focus on diabetes.
“I think diabetes surgery will become common within the next few years,” said Dr. John Dixon, the lead author of the study and an obesity researcher at Monash University in Melbourne, Australia, where the research was conducted.
The study and an editorial about it are being published Wednesday in The Journal of the American Medical Association.
The editorial, by doctors not involved in the study, said, “The insights already beginning to be gained by studying surgical interventions for diabetes may be the most profound since the discovery of insulin.”
A researcher who is not a surgeon and was not part of the research, Dr. Rudolph L. Leibel, co-director of the Naomi Berrie Diabetes Center at Columbia University Medical Center, said the study was important because it showed that a minimally invasive type of surgery could reverse diabetes.
“At this point,” Dr. Leibel said, “maybe we should be more accepting or responsive to the idea of surgical intervention for reducing or prevention of diabetes and its complications.”
But at the same time, he said, caution was in order, because the study lasted only two years and it would be essential to find out how these patients fared over time.
About 19 million people in the United States have Type 2 diabetes, and another 54 million are “prediabetic,” meaning they have abnormalities in their blood sugar that increase their risk for the disease, according to the American Diabetes Association. Diabetes is the fifth-leading cause of death by disease in this country, killing about 73,000 people a year. The number of cases in the United States is growing by about 8 percent a year, according to the association. Though treatable, the disease is not curable, and it is often poorly controlled.
The 60 people in the study had an average age of 47 and were assigned at random to have either surgery or medical care. All were obese, with a body mass index, or B.M.I., of 30 to 40. A B.M.I. over 25 is considered overweight, and over 30 is obese. (A person who is 5 feet 6 inches tall with a B.M.I. of 25 would weigh 155 pounds; with a B.M.I. of 30, 186 pounds; a B.M.I. of 35, 216 pounds; and a B.M.I. of 40, 247 pounds.)
Based on guidelines created by the National Institutes of Health in 1991, weight-loss surgery is generally only recommended for people whose B.M.I. is 40 or more, unless they also have Type 2 diabetes, in which case a B.M.I. of 35 is the cutoff. In this study, 13 people, or 22 percent, had a B.M.I. under 35.
Medicare covers weight-loss surgery according to the institutes’ rules, but many private insurers refuse to cover the surgery at all, said Dr. Philip Schauer, director of the bariatric and metabolic institute at the Cleveland Clinic. He said his center had to turn away three or four patients for every one accepted because insurers would not pay.
On average in the United States, banding costs $17,000 and the other bariatric operations $25,000.
Dr. Schauer said that the B.M.I. cutoffs did not make sense medically and that the study “blows away this arbitrary barrier.” He said that the cutoffs should be lowered, so that a patient with diabetes and a B.M.I. of 34.9 would not be considered ineligible, as is now the case.
Dr. Francesco Rubino, director of the metabolic surgery program at NewYork-Presbyterian/Weill Cornell Medical Center, also said that the criteria for the surgery should be changed so that it could be offered to diabetes patients early enough to reverse the disease.
Dr. Rubino and other researchers said that weight-loss operations that rearranged the small intestine had faster and more powerful effects on diabetes than did the banding, because the other operations changed the levels of certain gut hormones that greatly improve the body’s ability to control blood sugar, weight and lipid levels in the bloodstream. These operations, and the hormones responsible, have become the focus of intense research.
Dr. Dixon has received research grants and speakers’ fees from the company that makes the gastric bands, Allergan Health, and the company paid for the study through a grant to the university. But his report said the company had no influence on the design of the study, the data or their report.
The editorial writers said they had accepted travel grants from Allergan and other companies to attend a conference on diabetes surgery in Rome.
http://www.nytimes.com/2008/01/23/health/research/23diabetes.html








+(3).jpg)



.jpg)
+(3).jpg)


No comments:
Post a Comment